Household Expenditure on Health Phenomenally High in Delhi: Survey

Representational Image. Image Courtesy: AP
Forty-one percent of households in the national capital accessed private healthcare and 12% accessed both government and private healthcare services in the year 2019, according to a report on the State of Health in Delhi, published by Praja.org, a non-profit organisation.
As per the report, which was compiled after surveying 25,041 households in Delhi, 47% respondents accessed government facilities. However, the report points out, “This is not reflected in the overall household expenditure on health, which continues to be phenomenally high.”
The report says that despite the city having several facilities, affordability in healthcare continues to be a serious concern. On an average, households in Delhi spend 9.8% of their total incomes on health, which, if calculated according to per capita income as per GDP, is a total of Rs 1,16,887 spent per household on healthcare in one year.
Combining MCD and state budgets together, Delhi had a health spending of Rs. 6,590 crores in 2017-18 and Rs 8,549 crores were allocated for 2018-19. The disease burden in the city, however, continues to remain very high. The data for the past three years shows that even though Delhi has been able to tackle dengue and malaria, which have both shown significant reduction in number of cases, water-borne diseases such as diarrhoea and typhoid are still very rampant, reflecting a poor quality of water supply in the city.
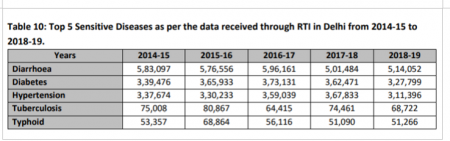
Between the years 2014-15 and 2018-19, the number of malaria cases in government dispensaries and hospitals decreased by 63%, from 7,723 to 2,874. The number of dengue cases have also considerably fallen after the 2015-16 outbreak when 27,119 cases were reported. For the year 2018-19, the number of cases was 6,699. The number of cases of tuberculosis has also gone down, from 75,008 in 2014-15 to 68,722. However, the number still remains very large.
Diarrhoea continues to be a huge health problem in Delhi, with 5,14,052 cases in the year 2018-19. The high number of diarrhoea cases reflects the poor quality of water supply in the city, which was also reflected in 36,426 water contamination complaints registered with Delhi Jal Board in the year 2018. Total cases of cholera in Delhi have decreased in the last three years, from 3,521 to 1,526.
According to the report, diarrhoea, diabetes, hypertension, tuberculosis and typhoid are the top five sensitive diseases reported in government facilities in the last five years. On an average, during this time period, people in Delhi have suffered the most from diarrhoea followed by diabetes. The report says, “It is an interesting point to note that there is not much change in occurrence of these diseases and no serious action has been taken by authorities to prevent these diseases to decrease their occurrences.”
According to the report, another huge cause of concern is the rising number of respiratory deaths over the years, which reflect the current public health ‘emergency’ that the city is grappling with. Air quality data collected by Praja through the Central Pollution Control Board (CPCB) shows that Delhi had only five ‘good’ Air Quality Index (AQI) days in the last four years (2015 to 2018). The average AQI levels in Delhi have been ‘poor’ in the past four years, with at least three months recording ‘very poor’ air quality.
A look at the data about respiratory diseases, which are caused and aggravated by air pollution, reflects a serious threat that Delhi’s residents face on a daily basis. In 2017, for instance, 551 deaths were caused due to cancer of respiratory and intrathoracic organs; 9,321 deaths were caused due to other respiratory diseases and infections. This comes to around 27 deaths per day in 2017, which were caused due to respiratory ailments and diseases, while this number was 33 deaths per day in 2016.
The report states, “A strong disease surveillance mechanism is key to monitoring public health indicators and in turn ensuring improved health of the populace. The capital city New Delhi, which in this regard could have been a leader for other Indian cities, is instead depicting a picture of an unaccountable and ambiguous monitoring culture of governance.”
For causes of deaths in the city, the data is available for institutional deaths only, which were 66% of total reported deaths in 2017. The report points out: “It is crucial to comprehend the data around causes of death to understand the severity of a disease. This can help the government to set policy agenda regarding which diseases need immediate attention and at the same time fixing gaps in the public health delivery mechanism.” Because this data is not available in a timely manner, health trends cannot be properly monitored in real time and neither can exigencies be preempted.
The report adds, “In spite of available infrastructure and a huge government spending, there is a poor evidence for its impact due to lack of a centralised monitoring mechanism and no proper structure for implementing healthcare policies.”
The mohalla clinic initiative for example, was started with the good intent of taking primary health at the community level and also providing affordable diagnostic services. According to the report, however, the scheme is not being properly monitored. It points out, “First, there is no uniformity in the way districts maintain this data. Secondly, the data for Mohalla clinics was not available with the Directorate of Health Services (DHS). Moreover, Mohalla clinics are not mandated to provide disease-wise data of patients to the Chief District Medical Officers, reflecting a poor disease surveillance in the city.”
It adds, “To improve the situation, it is crucial that the elected representatives become proactive and hold the government accountable for the city’s healthcare system. The government on its part needs to take strict policy action on the health determinants such as pollution and contaminated water. In addition, a uniform and transparent system needs to be put in place to provide public healthcare to the city with ease of access and affordability.”
Also read: Most Ayushman Bharat Claims Made in Private Hospitals, Says Govt Report
Get the latest reports & analysis with people's perspective on Protests, movements & deep analytical videos, discussions of the current affairs in your Telegram app. Subscribe to NewsClick's Telegram channel & get Real-Time updates on stories, as they get published on our website.
























