Budgeting for Universalization of Indian Public Health Care Sector: Lessons from Covid-19?
Limitation of Private Health Insurance in Covid-19 Pandemic
In 2018, September, the present Modi government launched the health insurance policy- Ayushman Bharat Pradhan Mantri Jan Arogya Yojana (AB-PMJAY) to cover health insurance of 50 crores people through PPP model. But, would it be viable to ensure universal public health care via adopting PPP model? The answer lies in the basic public economics principle of provision and production of public services, like health services. The private health services would not lead to a complementary relationship between efficiency, equity and social justice. After the completion of 2 years of implementation of the AB-PMJAY, there are reported cases of corruption, showing the failure of privatization in healthcare sector and wastage of public funding via adopting PPP model. The PPP model in the health care sector used insurance in the healthcare services by the government and private hospitals as 55% of total hospitals empaneled in the AB-PMJAY scheme are private and 49% of patients who claimed their insurance policy in 2019-20, got treatments in the private hospitals.
The V-shaped recovery in the number of claims, under health insurance policy-AB-PMJAY, highlighted in the Indian Economic Survey 2020-21 is projected as revival of normalcy in Indian healthcare services. This further propagates the significance of health insurance under PPP model rather than advocating the role of public health care in universalizing health care under Sustainable Development Goal- 3. As it states: “access to medical services were classified as essential services during the lockdown, care-seeking exhibited a V-shaped behavior during the lockdown and unlock phases with the pre-Covid-19 levels being reached in December 2020…we can observe a steep fall in claims under the overall general medicine category for PMJAY in the March -April 2020 period… Further, recovery in private sector hospitals is much better than the public empaneled healthcare providers (EHCP)” (MoF, 2021)
Market Failure
There is a catch in this V-shaped recovery as it reflects the market failure of the private sector in the provision of public good, viz., health services. Covid-19 experiences entail the horrific environment when private hospitals clearly shirked from their responsibilities of provision of health services to the patients. In a situation when the under prepared public healthcare was busy tackling the pandemic situation, private hospitals either refrained from or charged exorbitantly for their services. That led to under supply of health services to the patients and burdened the public sector hospitals. The public sectoral hospitals remained at the forefront in delivering the health services to contain and treat the patients of Covid-19 along with treating other patients. It was noticed that the private health care providers have been shirking from their social responsibilities as most of the private hospitals in India are not delivering more than 50% of their capacities of beds and patients’ intakes in the private hospitals during the Covid-19 pandemic. They are also withdrawing from delivering 10% quota of hospital beds for the Indoor Patient Department (IPD) and 25% reserved Outdoor Patient Department (OPD) quota of beds to the Economic Weaker Sections (EWS) of the society as the government gives the expenses of the health expenses of the EWS category.
Privatization
The private health care service providers and hospitals remain absent from the provisioning of health services in this health emergency. Rather there are instances of private hospitals making profit out of misery of the masses during Covid-19 pandemic by charging exorbitant medical fees. For instance, according to the media reports, the private Max Hospital in Delhi is charging Rupees 250 thousand for a Covid-19 package and the plasma therapy for the Covid-19 patient has been charged at Rupees 25 thousand by the private hospitals in urban India. Such episodes add on to enough reasons for arguing against private intrusion in social sectors mainly health and education. So, despite the pandemic being class and caste neutral, burden of medical expenses is exorbitantly high for poor people. But, later, during the unlock period, as condition of Covid-19 improved, then private sector hospitals became more active in normalizing their supply of health services to reap the profit.
The Economic Survey 2020-21 doesn’t acknowledge the market failures in the Indian health care sector, which was witnessed during the medical emergency. It is stated that the private sector including multinational companies are not interested to deal with global public health crisis like the Covid-19 pandemic but private hospitals and pharmaceutical companies are willing to accumulate more capital by undertaking more business with public health and maximize their profits by any means (Harvey, 2020). We can easily explain the processes of de jure or pure privatization of health services in India expanded since early 1990s, Indian government has also promoted the de facto privatization in terms of public private partnership (PPP) model.
Figure 1 also shows that comparative private, public and out-of-pocket health expenditure in India and nine other countries. Figure 1 shows that out of total 3.5% of GDP, Indian health care expenditure (lowest), private expenditure is highest at 73% at global level and the share of public health care expenditure is lowest at 27%. Conversely, the higher role of private health expenditure can also be explained by the out-of-pocket health expenditure in India, which is also highest at global level 62%. In comparison to the Indian case, the out-of-pocket health expenditure in China is lower at 36% out of total expenditure in health. Public funding by the Chinese government in healthcare is higher at 57% and private health expenditure is lower at 43%. This implies that the Chinese government spends more public funding on health than Indian government. On the other hand, the neighboring country- Pakistan also has higher health private expenditure, 68% and 32% of public expenditure, reflecting lower public funding and higher private expenditure. The out of pocket of health expenditure in Pakistan is 60%, showing near to equal shares of private and out-of-pocket expenditure in developing countries -India and Pakistan.
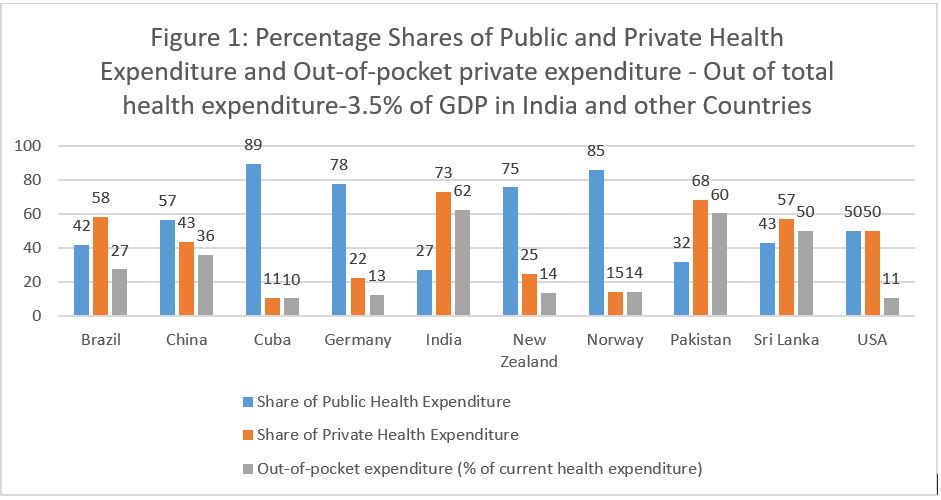
Source of Data: Figure constructed by using data of the World Bank – WB (2020)
Lessons from Covid-19 Pandemic for Universalization of Health Care
The health outcomes in India are poor at global level due to lower ratios of health professionals, and lowest public funding, which in turn reflect a crumbling situation of Indian health infrastructure. The condition becomes severe when private health care providers across the country are either making profits or shirking from their social responsibilities in the Covid-19 pandemic. The situation confirms the market failure in the provision of public good and so by allowing private stakeholders dominance in healthcare, the Indian government is violating the basic principles of the public economics since early 1990s under neo-liberal economic policies. The Economic Survey 2020-21 highlighted the importance of an increase in public funding from 1% to 2.5%-3% of GDP to universalize health care as the Indian Health Policy 2017 also promised this target of increasing public funding. At last, rather than reproducing the rhetoric, policy makers need to learn lessons from Covid-19 pandemic to ensure universalization of Indian public healthcare by strengthening the budgetary provisions of 3 per cent of GDP in the Budget 2021-22 by the central government.
Courtesy: VIKALP
Narender Thakur, University of Delhi [email protected]
Vaishali, National Institute of Educational Planning and Administration [email protected]
Get the latest reports & analysis with people's perspective on Protests, movements & deep analytical videos, discussions of the current affairs in your Telegram app. Subscribe to NewsClick's Telegram channel & get Real-Time updates on stories, as they get published on our website.