COVID19: What Do Mutation Studies of the Virus Reveal?
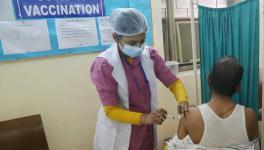
Representational image. | Image Courtesy: First Post
The world is way behind in curbing the COVID-19 pandemic. Achieving herd immunity naturally is far from reality and an effective vaccine is also not likely to be available in the near future. In such a scenario, the perhaps only remaining choice is to look at the mutation of the virus. Is there any mutation that the novel coronavirus (causing the pandemic) has acquired in its course of progression making it more severe or inhibiting its spread?
Surely, there are mutations that SARS-CoV-2 has undergone since its appearance last year. But six months into the pandemic caused by it, the analysis of the effect of the mutations, that could determine whether it is deadlier or benign, unfortunately, remains inconclusive. One of the reasons behind this is that the virus undergoes mutation slowly in comparison with the other viruses. On average, the virus adopts two changes per month, meaning in its entire genome of about 30,000 base pairs, changes in two positions take place. Most of these mutations don’t lead to any change in how the virus behaves, but a few might cause a good difference in either severity of the disease caused or the transmissibility of the virus.
Why the virus mutates comparatively slowly is still an unanswered question in front of the scientific community. Some put forth the hypothesis that SARS-CoV-2 had already acquired the changes required for its good adaptation in the human body at the very beginning when it jumped over to the humans. The virus is now well equipped to keep on spreading and hence does not face evolutionary pressure as such.
One of the earliest evolutionary evidence in terms of gene changes was reported in March by Lin-fa Wang et al of the Duke-NUS Medical School, Singapore. It is available on the preprint server biorxiv. The change was a deletion of 382 base pairs in the gene ORF8. The function of the gene, however, is unknown. This genomic change was reported from Taiwan as well. Interestingly, deletion in the same gene was also seen in the SARS-CoV which caused the 2003 outbreak. In SARS, lab experiments later showed that the mutated variant was less efficient in replication, hinting that the mutation could have slowed down SARS. However, in the case of SARS-CoV-2, the same mutation may not have the same benign effect as in SARS, cell culture experiments in the lab suggest. Nevertheless, the possibility of milder disease due to the mutation cannot be ruled out totally, according to Wang.
The latest finding on a mutation has drawn some attention—the mutation at the position 23,403. The report published in Cell, about this mutation claims that the viral strain carrying this mutation is now widely circulated across the world and apparently has become the dominant variant, outnumbering the earlier strains.
This mutation is also important in another aspect; it has led to a change in the spike protein of the virus. The spike protein on the surface of the viral particle helps the virus cling on to human cells and eventually enter. The mutation has changed the amino acid at position 614 of the spike protein from a D (aspartic acid) to a G (Glycine). This is why the mutation is called G614.
Also read: Laos Has Tackled COVID-19, But It Is Drowning in Debt to International Finance
Can it be said that this change has caused a milder disease? According to Kristian Anderson, a computational biologist at Scripps Research, “Any one mutation may rise to very high frequency across the world, just because of random chance. This happens all the time.”
The COVID-19 Genomic Consortium of the UK has found that the G614 variant spread 1.22 times faster than the D variant. The consortium sequenced 30,000 genomes of the SARS-CoV-2. The Cell paper also said that the G variant is more infectious and the viral loads are also found to be higher than the original D strain. Nevertheless, this does not increase the severity of the disease. They have also turned to lab experiments with cell cultures where they have found that the G variant is more efficient in entering the cell than the D one.
University of Massachusetts Medical School’s Jeremy Luban also found similar results. The G614 confers a slight change in the shape of the spike protein which eases the fusion of the viral spike protein with the human cell surface. Luban and others’ experiment shows that the G variant is 3 to 6 times more infectious.
However, all these experiments are conducted on cell lines. The findings on cell lines may not replicate as such in real life situations inside the body. In laboratory cell lines, there is only a specific type of cell that the experiments are carried on. But, the human body has a vast array of cells, including the immune cells, and what we get in a lab cell line may not exactly translate in the human cell milieu.
To probe whether the dominant G variant, which was absent four months back, can actually cause greater transmissibility of the novel coronavirus in real life, one way is to conduct experiments on animals. In it, animals like ferrets or monkeys have to be exposed to the D and the G variants and then see how much virus they shed in the case of each variant. Interestingly, in Dutch mink farms, the virus has transmitted from humans to the minks at different times. Out of five times the virus was transmitted to the minks from humans, twice it was the D variant while thrice, it turned out to be the G variant.
However, the present data shows that the G variant has somehow managed to outnumber the D variant globally. If this truly indicates greater transmissibility of the virus, but with less severity, then it could mean something better for the people. But, more evidence is needed to come to such a conclusion. Moreover, it can be useful from a vaccine point of view. When a specific strain dominates the world, vaccine production could be focussed on that variant.
Get the latest reports & analysis with people's perspective on Protests, movements & deep analytical videos, discussions of the current affairs in your Telegram app. Subscribe to NewsClick's Telegram channel & get Real-Time updates on stories, as they get published on our website.