COVID-19: Testing Continues to Drop Amid Rising Cases of Infections in Delhi
Image Courtesy: Reuters
Neha Yadav (changed name) reported to work after the administration of the private broadcaster where she works told its employees to resume work amid the increasing cases. However, she has met with the unpleasant news that she dreaded after joining back. Seven colleagues complained about sudden fever and other related symptoms. When they consulted doctor, the doctor suggested them to go for COVID-19 test. Yadav's experience at two government hospital reveals a telling experience about the poor patients who cannot afford COVID-19 tests at private facilities.
Sharing her experience with NewsClick, Yadav said, “The senior managers first tried private laboratories to get us tested but every lab declined to conduct tests owing to ban imposed by the government. When all our hopes extinguished, we were told to go to LNJP hospital. We reached hospital at 9:30 AM. There was no one to assist us for test. We were forced to run from one counter to another to get all clearances. By 12:30 PM, when we got clearances, we were told to come next day as the hospital took samples till 11 AM only. Considering the arrangement and increased risk of infection, we moved to Lady Hardinge Hospital for tests. After standing in queue for seven consecutive hours on June 7, we were finally tested. On June 9, we were informed that all of us were positive."
Yadav's harrowing experience, from complete denial by private labs to limited testing at government hospitals, shed some light on the consistent under-testing in the national capital. On May 28, 7,615 patients were tested which came down on June 1 to 4,753. After witnessing some momentary surge, the numbers eventually came down to 3,700 on June 8. Interestingly, the ratio of infected persons to number of tests conducted increased sharply during the period. An analysis by the NewsClick data analytics team suggests a rolling seven day average of infected persons started increasing from May 24 itself. On May 24, the ratio was recorded 9.87% which reached 14.98% on May 31. The surging figure continues till date when 25.45% of tested persons turned positive on June 10.
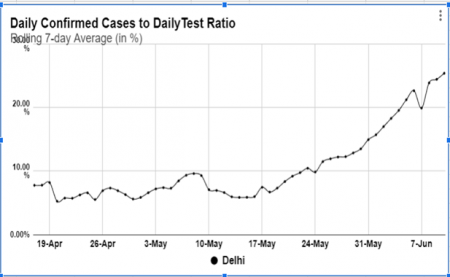
But why did the number of tests conducted consistently come down? Reports argue that the decline came with the government imposing ban on eight leading private laboratories who started testing asymptomatic patients. While the Indian Council of Medical Research suggested a generous testing, Delhi Government's order limited testing to high risk patients with comorbidities, frontline workers showing symptoms of COVID-19 and all patients affected with Severe Acute Respiratory Infection and barred asymptomatic patients.
The restriction remains a perplexing move given the latest statement of Delhi Health Minister Satyendra Jain about community transmission. Recently, Jain had accepted that 50% patients were not aware about their source of infection. Testing asymptomatic patients remains a crucial tool in breaking the chain of infection as they unknowingly become the carriers of infection to their communities.
However, a conversation with an advisor to Delhi Government sheds some light on limited testing. The advisor, who requested anonymity, said, “The increase in tests reflected when the private hospitals started testing every patient seeking admission for treatment. Their concern was understandable because any infected patient has the potential to infect others and turn a place into hotspot but what was more perturbing that the private laboratories started making all sorts of excuses like contamination of samples and charged them twice. We received a number of such complaints. Thus, we decided to put a brake on it." Interestingly, this advisor also said that the approach of ICMR and other government agencies is more directed towards achieving herd immunity than preventing the spread of the virus.
Harjit Singh Bhatti, Senior Geriatrician who served at AIIMS, maintains that the lower number of testing signifies no change in attitude to health scenario in midst of the pandemic. Talking to NewsClick, he said, “This approach simply suggests that the government is still thinking that the patients will come to hospitals and the doctors will treat them. We call this self-defeating approach sick care because it's more concerned with treatment than prevention. It is this approach that stopped the development of primary and secondary care sector in healthcare and hospitals were projected as one stop solution. Unfortunately, it does not work that way. Second, I think what could be reason behind limiting testing is that the government failed to act swiftly during the initial lockdown. It could have ramped up the testing, built temporary hospitals, procured testing kits but it did not. Now, you need isolation centres to put people there once they are found positive but there are none. It is depending on home isolation. Thus, with the limited testing, it wishes to save its face but unfortunately that’s not how pandemics work."
Get the latest reports & analysis with people's perspective on Protests, movements & deep analytical videos, discussions of the current affairs in your Telegram app. Subscribe to NewsClick's Telegram channel & get Real-Time updates on stories, as they get published on our website.
























