Covid-19: Which Indian States Failed Miserably in Tackling the Pandemic?
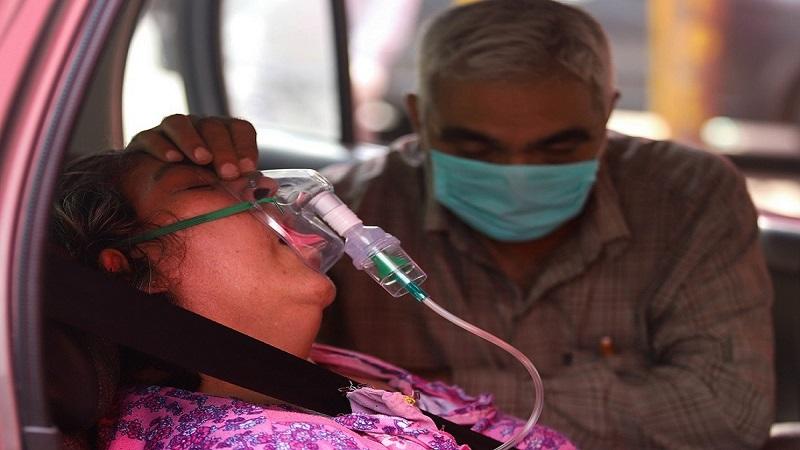
Image Source: Vijay Pandey
The second wave of the Coronavirus pandemic has surely been aggravated by a casual attitude towards world trends and an absence of preparedness overall. Election rallies and religious gatherings where hundreds of thousands gathered unchecked were allowed. The second wave has been reportedly fueled by two variants- B.1.617 (that was first found in December, 2020 that spread through mass events) and B.1.1.7 (identified first in Britain that reached India through travelers). The former variant has ravaged India, and we are witnessing the worst of it.
India, painting a bleak picture
As of now, the country is facing shortages that are enormously adding to its Covid-19 woes. Shortage of oxygen, medicines, beds, ambulances, crematoria/burial ground space, ventilators, medical staff, food, jobs and lifesaving vaccines. This, with copious amounts of hoarding, black marketing, PR exercises to sustain a global image has proven to be more disastrous than the virus itself.
An Open Data Tracker suggests that over 512 people in India have died due to oxygen shortage in hospitals between April and May 16. It does not include the ones that died waiting for beds and oxygen outside hospitals. The publicly available tracker estimated that the highest number of oxygen related deaths (83 deaths) took place across five medical colleges in Goa. Karnataka reposted 54 such deaths till May 16, including 36 persons at Chamarajanagar Institute of Medical Sciences, 4 patients at KBN Hospital at Kalaburagi, 2 patients at Arka Hospital in Bengaluru, 5 at Shri Bhanji D Khimji Lifeline Hospital in Hubballi, 4 at Kalaburagi government hospital and 3 at Belagavi government hospital.
Moreover, under reporting of deaths across the country has been widely reported in international news media as well. A New York Times report of May 25 states that the official count as of May 24 has been of over 3.07 lakh deaths (at 3,07,231) while in a ‘more likely scenario’ deaths are likely to be over 16 lakhs (1.6 million) and in a worst case scenario, the deaths could be 42 lakhs (4.2 million). The reports states that despite India recording largest daily death toll in third week of May, it is still most likely an undercount. Speaking for world figures, a report by the World Health Organization (WHO) estimated that the global death toll of Covid-19 may be two or three times higher than reported.
Unsurprisingly, the attention and focus on rural areas have remained acutely absent. To put things into perspective, rural India constitutes a massive portion of India with a whopping 65.53 percent of the total population. This means 89,53,86,226 people. To narrow it down even further, for instance, the Patna High Court recently looked at the district wise breakup of the population living in urban and rural areas in Bihar, which revealed that almost 90 percent of the population resides in rural areas. The pandemic has clearly exposed the reality of the crumbling healthcare infrastructure in urban, so called developed areas. The rural space can be just left to one’s own imagination!
An outbreak like such, goes beyond the framework of public healthcare systems. It involves, and especially in context of a nation this hugely populated, a concrete nexus of Centre-State cooperation, resources, long term strategy planning and instantaneous action. Overall, some states have fared better in managing this crisis, while some States have despairing accounts of tragedy one cannot march on from.
The Prime Minister, while campaigning in Asansol (West Bengal) in April, said that he was elated to see the large crowd that had gathered at his rally, on a day when India recorded 2,00,000 cases and over 1,000 deaths. He forgot to mention how notoriously fragile his Indian state is. The GOI justified the lockdown in March 2020 to ramp up the infrastructure to deal with Covid-19. Whatever little that was done under the garb of one of the strictest lockdowns in the world, has remained calamitously marginal. More so, the government in 2021 is clearly more underprepared than it was in 2020.
The residents of Uttar Pradesh, Gujarat, Bihar, Delhi now explicitly feel abandoned by their respective governments manifested through begging and pleading for basic facilities. The floating images of death in the Ganges shows how India is not counting its dead. These states have had ambulances turned away for lack of space, people dropping dead while gasping for air and Covid patients perishing to hospital fires. Even Delhi had the shocking visuals of dead bodies of near and dear ones being lined up at crematoria and burial grounds.
Here is a closer look of states that have failed to uphold its citizens’ basic right to health with its chronically under resourced healthcare system.
Delhi
All of 1,484-kilometre square of space, and people in the National Capital could not find space to bury their dead. Delhi was forced to build makeshift funeral pyres. The public health expenditure on Delhi between 2020 to 2021 has been Rs. 7,704 crores with approving Rs. 2,578 crores for upgrading and expanding 16 hospitals. In the 2021 budget, Delhi announced the allocation of Rs. 9,934 crores, which amounts to 14 per cent of the total outlay for the health sector.
With a landslide victory in 2015, the Arvind Kejriwal led Aam Aadmi Party (AAP) promised developments in areas like public health care and education. The Delhi Government had proposed a three-tier structure- Mohalla clinics, poly clinics and hospitals. It proposed around 1,000 Mohalla clinics and 125 Poly clinics. But overall, Delhi only has 450 Mohalla clinics and 25 Poly clinics. As this model was widely praised by other states and also got international coverage and praise by former UN Secretary-Generals Kofi Annan and Ban ki-moon. But this too seemed inadequate to tackle Covid crisis.
Further, the government reduced the allocation for the development of Mohalla clinics and polyclinics from Rs. 403 crores in 2018 to 2019 to Rs. 375 crores in 2019 to 2020. According to ThePrint, AAP’s promise of creating 900 Primary Health Centres (PHCs) and adding 30,000 beds to Delhi hospitals have not been met. According to Government data from September 2020, Delhi only has mere 540 Primary Health Centres.
When Delhi residents scrambled for beds and oxygen, the High Court had pulled up the government several times for its laxity. Recently, the government was hammered by the High Court for providing inaccurate information on the availability of a 250-bed Covid-19 facility in one Indira Gandhi Hospital in Dwarka, reported LiveLaw. The court was livid as the government assured it that the facility was up and running but in reality, did not admit one single patient even after 72 hours.
Noting that the entire medical infrastructure has been exposed during the pandemic, the Delhi High Court had also opined that the entire system had failed in its duty to provide adequate medical assistance to its residents. The shifting responsibility between the AAP government and the Union government continued in courts with hospitals sending SOS calls for oxygen. On one hand where the state government kept yearning for more oxygen, Centre argued that they are supplying enough but the quantity is not reaching hospitals due to shortage of cryogenic tanks.
The Delhi High Court and the Supreme Court repeatedly pressed and eventually ordered (strictly) that Centre supplies the demanded quantity to Delhi on a regular basis but also pulled up the state government for not taking systematic steps for procuring cryogenic tanks for oxygen and make adequate security arrangements for their movement to various Covid-19 hospitals.
Amidst this conundrum of supply chain management, lives were lost. Twelve Covid patients including the gastroenterology department’s head died in Batra Hospital due to oxygen shortage today on May 1. Jaipur Golden and Sir Ganga Ram Hospitals have lost 25 patients each similarly, in April.
A Right to Information (RTI) activist, Vivek Pandey had filed an RTI seeking information about oxygen plants in Delhi. Despite the Delhi government purchasing 4,500 oxygen cylinders and tanks between July 2020 and April 2021, the capital city did not install enough oxygen plants or engage adequate number of oxygen tankers on time to supply to hospitals. The government, as per the RTI query, also revealed that Delhi did not order or purchase any ventilator between July 2020 and April 2021.
Currently under lockdown, Delhi seems to have crossed its peak with nearly 7,000 cases in the past 24 hours, but with cases even testing seems to have dropped from 70,000 per day to around 60,000.
Uttar Pradesh
The state has recorded over 16.8 lakh cases and over 19,500 deaths as of May 24. Mathematicians and date management experts worldwide have projected that India’s deaths could well be three-five times higher than officially admitted figures.
According to the latest budget released by the State of Uttar Pradesh, Rs 5,395 crores has been allocated towards National Rural Health Mission and Rs 1,300 crores has been allocated to Ayushman Bharat Yojana. The revised budget towards the Health and Family Welfare department was Rs.20,582 crores in the year 2020 to 2021 and Rs. 32,009 crores in the financial year 2021 to 2022.
A state with the highest percentage of rural population, with approximately over 15 crore people, constituting 18.62 percent of the country’s rural population, has only 2,936 PHCs. According to PRS Legislative Research, in 2020 to 21, payment towards salaries and pension decreased by 20 percent. The estimated budget was Rs. 1,36,988 crores and the revised amount fell to Rs. 1,09,914 crores.
At the Jhansi Medical College in Uttar Pradesh, the nursing staff had not received their salary for seven months. On 25 March, 2020, with Covid-19, they boycotted work for the day. In an interview to the Caravan, one nurse said that she met a member of the administration who asked them to “cooperate.” She said she told the administration, “We have been cooperating for seven months now. Corona has just appeared on the scene, a month, or a month and a half ago. It hasn’t been around for seven months, right? Then why are you not paying the salaries? Give it to us after two months, but at least give it.”
As per the media, Chief Minister Ajay Bisht alias Yogi Adityanath announced an increase in the salary or honorarium of all healthcare and frontline workers including doctors, paramedical staff, housekeeping staff, sanitation workers, accredited social health activists and Asha, Anganwadi workers. This announcement came a week after Etawah district’s biggest government hospital, BR Ambedkar Hospital, struggled to cope with lack of staff.
According to an IndiaToday report, the bathrooms in the 100-bed Covid ward were locked after sanitation workers said they would not work in Covid wards. No one from the hospital administration or even medical staff were present in the premises. The families of patients have been forced to open oxygen cylinders.
While addressing the media recently, Yogi Adityanath said within 10 days, active cases have dropped and the situation in the State is ‘under control’, when in actual fact –due to coercion and threat of penal action, more than 1,000 primary and upper primary school teachers on election duty have succumbed to the virus.
The Government’s idea of creating a portal to show availability of Level-2 and Level-3 beds in Covid wards and ICUs in various hospitals within the state failed too, as it displayed incorrect data. The Allahabad High Court criticised the affidavit submitted by the government while noting that albeit the portal showed availability of vacant beds, no hospital could offer any, “This state of affairs that we have come to know about the management of online portal created by the Government today casts shadow upon the Covid Hospital Management,” opined the court.
The vindictive government in UP is asking its citizens to quit complaining. Intimidation, arrests, FIRs for spreading ‘panic’ if raised alarms about oxygen or storage capacity have been the tools adopted for crisis management. On May 11, when the High Court continued to hear the suo motu matter on Covid management and through the government’s affidavit it found that:
-the proper procurement and supply of the life savings drugs/ life support systems like BiPaP machines and High Flow Nasal Cannula Masks have not been made available to the various hospitals
- number of testing has been reduced gradually
- details regarding oxygen production in the State qua 22 hospitals have not been given
- the availability of ambulances with advance life support system is also very less considering the number of districts in the State
- Rs.100 is allocated per patient in Level-1 category hospital despite knowing that Covid patients need highly nutritious food of about 2100 calories in a day
- No details have been given regarding Level-2 and Level-3 hospitals.
UP seems to be at a juncture of systemic failure at each level.
Gujarat
As per reported data, the state has had 7.9 lakh cases and over 9,000 deaths as of May 24. Mathematicians and data management experts worldwide have projected that India’s deaths could well be three-five times higher than officially admitted figures.
Gujarat is among the states which has been notorious for under reporting deaths. On April 27, 2021 Gujarat’s local newspaper Sandesh set aside five pages for obituaries in the Rajkot edition alone, while the state’s Covid-19 dashboard recorded only 14 deaths in the previous 24 hours. Thus, making obituaries better indicators of death count in the area, rather than official data. On the same day, the newspaper stated that 87 bodies were cremated following Covid protocol over the last two days while the government only recorded two Covid deaths.
City-wise, the highest disparity during this time was in Gandhinagar that reported three official Covid deaths even though 80 bodies were cremated as per Covid protocol. Similarly, Jamnagar cremated 208 bodies as per Covid protocol but the official data only acknowledges 23 Covid deaths. In Rajkot, 124 bodies followed the protocol but only 27 Covid deaths were reported. There have been reports of people waiting in queues outside crematoria to cremate their loved ones as well as outside burial grounds. On April 13, multiple publications including The Times of India, The Telegraph, Hindustan Times and a few others carried a report by the Press Trust of India (PTI) about how frames of furnaces at two Surat crematoria had begun to melt under pressure as bodies were being cremated round the clock. However, official data constantly defied such reality on ground, gaslighting the media and the public at large.
A report stated that Gujarat issued about 1,23,000 death certificates between March 1 and May 10, however during this period only 4,218 Covid deaths have been recorded. Further, a fairly recent report in The Hindu, of May 16 suggests that official data of number of deaths emerging from rural and remote districts were about 20 times lower in some districts.
The High Court took stock of the situation in the state while noting at the outset that the state seems to be in an “health emergency”. As of May 18, Gujarat has recorded over 7,60,000 cases and 9,200 fatalities. In this year’s budget for the financial year 2021 to 2022, the government allotted Rs. 11,323 crores towards the health sector. Comparing this budget estimate to the previous year’s revised estimate, the Gujarat government’s expenditure on the health sector has actually dropped to 5 percent from 5.2 percent.
Based on the National Health Policy report (2017), that aims at informing, clarifying, strengthening and prioritising the role of the Government in shaping health system, stated that the current financing to the health sector needs a push. It suggested “Increase health expenditure by Government as a percentage of GDP from the existing 1.15% to 2.5 % by 2025” and also increase the state sector health spending to more than 8 percent of their budget “by 2020”. Despite this recommendation, the percentage remains consistently low at a 5 percent.
Gujarat has hardly seen an increase beyond six percent in the health sector. Perusing the past expenditure on healthcare, the percentage of total budget Gujarat has spent on health has been abysmally low. As projected by a Times of India report, the state data shows:
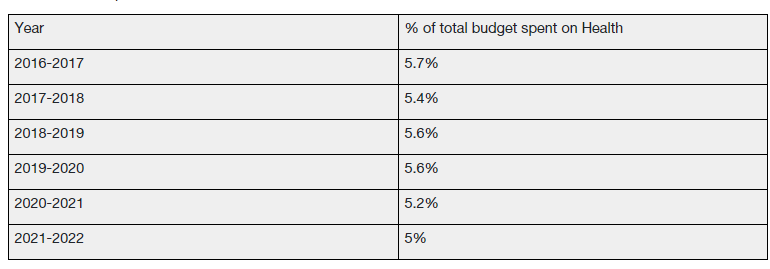
Despite having faced major challenges in the health sector because of the pandemic, Gujarat is lagging behind. The state’s budget to the nutrition and social welfare has also plummeted to a minus 23 percent. The revised estimate in the financial year 2020-2021 was Rs. 9,293 crores and the budget estimate for 2021-2022 stands at Rs. 7,160 crores.
India’s so called ‘model state’ had ambulances turned away from hospitals for lack of beds. It suffered from massive under reporting of Covid-deaths. Bhaskar reported on how from March 1 to May 10, within a span of 71 days, around 1,23,000 death certificates were issued but the government concealed this number and recorded only 4,218 deaths. The non-transparency was so apparent that the high court had to intervene to order the government to be honest about Covid-19 data.
Bihar
The state has had about over 6.96 lakh cases and over 4,700 deaths as of May 24 Mathematicians and data management experts worldwide have projected that India’s deaths could well be three-five times higher than officially admitted figures.
Bihar’s Covid stories hit even harder after apocalyptic images of saffron pyres on the river banks and bloated bodies in Ganga emerged. The projected population of Bihar is 13.12 crores. For 13.12 crore people, Bihar managed to construct only 1,994 PHCs, out of the allotted budget of Rs. 5,766 lakhs between 2019 to 2020, as per government data.
Further, as per the recent budget for the period 2021 to 2022, the Bihar government set aside Rs. 360 crores towards incentives to ASHA workers. But according to a NewsClick report from May, ASHA workers have been persistent in their demand for Rs. 10,000 as honorarium and state employee status to ASHA facilitators over the past few years, but none have paid heed to it. Despite several protests at PHCs across Bihar, the government has turned a deaf ear to their demands.
Even though ASHA workers have remained prompt from day one of the pandemic, regular honorariums and expecting Covid incentives is a distant dream with some workers not having had received 16 months of payment in the State. As per reports, health sector has been devoted about Rs.13,264 crore this year.
The NITI Aayog Health Index report (2019) illustrates the deterioration of Bihar’s overall performance between 2015-16 and 2017-18, with a fall in many sectors such as sex ratio at birth, fertility rate, low birth weight, staff nurse vacancies and fully functional PHCs (mere 1,994). Bihar saw the highest decline of 6.35 points from 2015-16 to 2017-18 in the health index amongst larger Indian states.
Bihar’s low nutrition levels have made the impact of the pandemic worse. According to National Family Health Survey (2015-2016), 48 percent of children under the age of five are stunted, whereas, 21 percent are wasted and 44 percent are underweight. More than two-fifths of women (42%) and 38 percent of men are either too thin or overweight or obese. More men and women are thin than overweight or obese.
Despite repeated directions to the state on medicines, testing, other infrastructural issues, most of them have remained on paper. For instance, during a hearing on 4 May, the court pointed out that on April 23, the government had assured it that 60 oxygen beds at ESIC Hospital, Bihta were being enhanced to 500 beds. However, on May 3 the court was informed that the State Government has not been able to ensure proper utilisation of even 60 oxygen beds, let alone enhancing the number of beds.
Bihar was also in a complete state of mayhem with allowing unregistered hospitals to run as Covid designated hospitals. The Patna High Court has also pulled up the government for providing contradictory information about oxygen supply, beds and other Covid related facilities and directed it to come clean. In the beginning of the second wave, ambulances carrying patients were asked to return from hospitals for lack of amenities.
As early as April 18, reports came in that Bihar hospitals were suffering oxygen shortage for a week. The Bihar chapter of Indian medical Association (IMA) had lodged a protest over the government’s mismanagement of Covid treatment in hospitals. Ten days later, reports came in that on April 25 four people died of oxygen shortage while one died due to lack of medical attention; there were also reports of hospitals asking patients’ families to arrange for oxygen cylinders themselves. As of April 28, as many as 16 private hospitals had only a day’s stock of oxygen left and in both private and government hospitals there a total of 900 ventilators throughout the state.
Further, Bihar also tops number of deaths of doctors as per the Indian medical Association, followed by UP and Delhi. 90 out of 280 doctors who have died across India are from Bihar.
There has also largely been misreporting in number of deaths. Between 1 April and 13 May, 2,579 last rites of Covid-19 victims were held at the four crematoriums and one Muslim burial ground within the limits of the Patna Municipal Corporation (PMC). However, the overall Covid-19 deaths during the same period stood at just 2,092, which is 487 less than the figures shared by the four crematoriums and one burial ground in Patna alone.
All such data points expose not only the mismanagement and lack of governance but also the clandestine attempts made by the state to hide its faults and paint a rosier picture reflecting poorly on the performance of the government and its handling of a pandemic.
Conclusion
With Prime Minister Modi’s victorious declaration at Davos for having “saved humanity from a big disaster by containing corona effectively”, India’s stark reversal on ground has shaken two things- people’s trust and Modi’s own image. As a federal set up, Indian States are mandated to cooperate with the Centre on response and action but they too are to be blamed for this shortcut to public health.
Courtesy: Sabrang India
Get the latest reports & analysis with people's perspective on Protests, movements & deep analytical videos, discussions of the current affairs in your Telegram app. Subscribe to NewsClick's Telegram channel & get Real-Time updates on stories, as they get published on our website.
























