Jammu: The Chaos Behind ‘All is Well’ as COVID Cases Spurt

Image credits: Raman/Jammu
The sub-district hospital in the Ranbir Singh Pura sector, popularly known as RS Pura, of Jammu district is the lone hospital for almost 200 border villages. Despite this, the hospital is unable to respond to any COVID- related emergency situation because it lacks the requisite equipment.
At the hospital, only rapid antigen tests (RAT) are done, and if a person tests positive and is in a bad condition, s/he is referred to Jammu's GMC or CD Hospital.
“This is a community health care facility masquerading as a hospital, and it is in disarray. There is no oxygen or ventilator. We have no facility to treat patients. We just conduct rapid tests. Even PPE (personal protective equipment) and gloves are not available to all staff,” a health worker at the hospital told NewsClick.
In Trewa village near the international border in Jammu’s Arnia sector, sarpanch (village head) Balbir Kaur is dialling one number after another seeking permission to build another quarantine facility this time. Last year, Kaur was hailed by Prime Minister Narendra Modi during his monthly radio show “Mann Ki Baat” for setting up a 30-bed quarantine centre.
“The situation is grim. The primary health centre in my village is defunct. Initially, there were RAT test camps but now these are no longer there. And until their condition doesn’t worsen, villagers don’t go for testing or hospitalisation because it is too far away,” said Kaur.
Even a year after the first wave of COVID-19 hit the Union Territory of Jammu and Kashmir, infrastructure constraints coupled with shortage of equipment at the sub-district hospital and primary health care centre in the border villages of Jammu reflects the lack of preparedness by the administration to deal with the current pandemic crisis.
The Jammu division, which comprises 10 districts, has witnessed a spike of 2000% active COVID cases since April 1 last, the official data suggests. It is to be mentioned that the deadly second wave of Coronavirus has been wreaking havoc on the South Asian subcontinent since the first week of April.
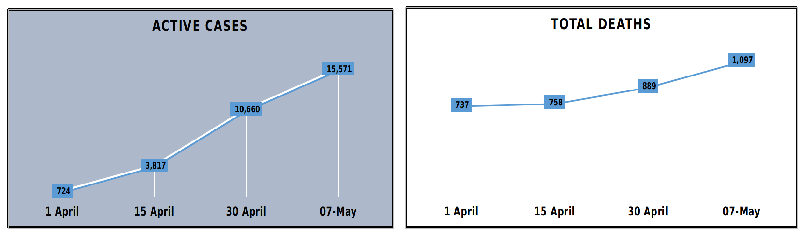
(Data credits: Pulkit Sharma)
The data released by the J&K administration on April 1 showed 724 active positive cases in Jammu division, which has risen to 15,571 by May 7, while the total deaths due to COVID-19 have seen a sharp increase of almost 50%, from 737 on April 1 to 1,097 on May 7.
Abdul Qudoos Bhat, 49, died at the District Hospital in Ramban district of Jammu division after he was denied oxygen despite repeated requests by his family members. According to Shaqat Bhat, a worker at his shop, who was present on the scene, Qudoos complained of breathlessness at 6 a.m when no doctor was present in the department. Shaqat then went downstairs to seek assistance from another health worker, but his request was denied.
“The other physicians and health workers refused to listen to us, claiming they were not informed about the case. This lasted two hours, and he died in front of us,” said Shaqat.
An investigation has been initiated, according to Shaqat, but the family is too devastated to even pursue the case. Not a single COVID ICU bed is available in the District Hospital of Ramban, which has already seen 31 deaths, as per data available on May 7.
The second wave of coronavirus has pushed the healthcare system past the breaking point in the Jammu region of J&K. The sub-district and district hospitals don’t have RT-PCR testing facilities, the ventilators donated under PM CARES funds are yet to be operationalised, oxygen plants have not yet been set up. As a result, the burden on the referral hospitals in Jammu district has increased. On Friday, NewsClick had reported how patients were seen lying in parks, ambulances, cars and on the staircases with oxygen cylinders at the premises of the Chest and Disease Hospital, the first contact point and triage facility for COVID patients in Jammu, all due to shortage of beds.
Asif Khan, a resident of Poonch district, says he has been waiting for his RT-PCR test results since the past four days. Khan claims his test was sent to Rajouri district, 87 kilometres away. The swabs of RT-PCR patients are sent to Rajouri district from Poonch due to the lack of RT-PCR testing facilities in Community Health Centres (CHC) and District Hospitals (DH).
“My rapid test results came negative but I had mild symptoms so I went for RT-PCR,” he adds.
There have been documented cases of viruses eluding tests, and delays in results that increase the risk of virus transmission. If not controlled, transmission can wreak havoc on rural populations that live farther from hospitals than their urban or suburban counterparts.
In Mendhar Tehsil of district Poonch, 60 kilometers south of the district headquarters, five ventilators are lying defunct. When asked, Satish Sharma, a resident and member of the Bharatiya Janata Party says no doctor is available.
“There are five ventilators in the Community Health Centre of Mendhar but these are yet to be operationalised because there is no doctor who can operate these,” he says.
As per available data, no COVID ICU beds are available in the Community Health Centre Mendhar, however, two ICU beds are available in the District Hospital, Poonch. It takes more than two hours reach Poonch from Mendhar tehsil, and four-five hours if you live in a remote village. Poonch has 772 active cases, as of May 7.
Meanwhile, official statistics show that there has been a sharp increase of 2114% in patients on oxygen support in the Jammu division, from 42 patients on April 15 to 930 patients on May 7.
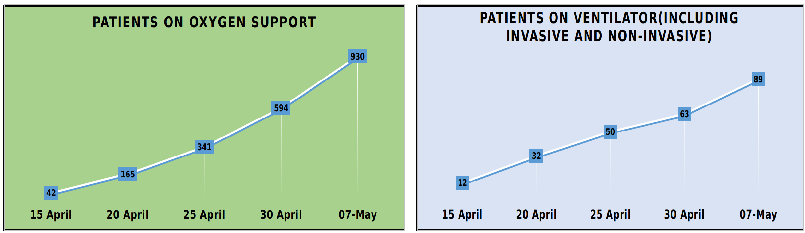
(Data credits: Pulkit Sharma)
An increase of 650% has been recorded for patients on ventilators, from 12 patients on April 15, to 89 on May 7. However, there has been a 12-fold increase in patients on invasive ventilator.
Smaller hospitals in other districts of Jammu division are also struggling to provide for COVID-19 patients who need oxygen or ventilators. An activist from Rajouri district’s Sunderbani told NewsClick that a majority of ventilators delivered to government hospitals are not yet operationalised.
Government data shows nine vacant COVID ICU beds at Government Medical College, Rajouri, 70 kilometres from Sunderbani. “The sub-district hospital had received five ventilators last August but these have not yet been put to use. Also, there are no rooms or personnel to operate the ventilators,” the activist, a resident of Sunderbani, said while requesting anonymity.
Rajouri district has 2,075 active cases, the second-highest after 7,087 active cases in Jammu district, as per the data on May 7. There are only five vacant COVID ICU beds out of 138 beds available as of May 7 in Jammu district, which is already witnessing an influx of patients from other districts.
The surge in the positive cases has created fear among people. A day ago, local residents protested against the administration’s reported decision to transfer oxygen cylinders from the District Hospital in Reasi district to Narayana, a private hospital near Katra.
The protestors were concerned that the shifting of oxygen cylinders would leave them with no oxygen. “We are poor people. We will go to a government-run hospital if we get infected with corona because we cannot afford a private hospital like Narayana,” said a protestor.
NewsClick tried reaching the Block Medical Officers (BMO) and Chief Medical Officers (CMO) to understand the reason for the poor infrastructure. But the officers were reluctant to speak.
One BMO told NewsClick that they had received instructions from the administration to not answer queries from any journalist. “I understand you are doing your duty. But I am also doing mine. I can’t even a say yes or no. We have been given instructions” the officer said.
Note: Comment from the administration will be updated as and when it is received
Get the latest reports & analysis with people's perspective on Protests, movements & deep analytical videos, discussions of the current affairs in your Telegram app. Subscribe to NewsClick's Telegram channel & get Real-Time updates on stories, as they get published on our website.
























