‘Not Hollow Glorification, Nurses Need Care, too’
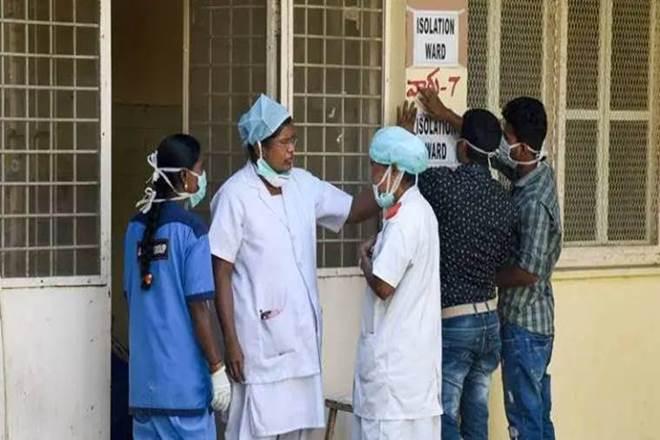
Representational image. | Image Courtesy: The Financial Express
Usha Devi, President of Kerala Nurses and Midwives Council, was in the thick of the Nipah virus challenge last year, as well as the ongoing COVID-19 battle in the state, which has received global appreciation. In an interview, Usha Devi says Kerala has come out with flying colours because of a strong, decentralised, people-oriented health system in place. Edited excerpts:
SC: Today, a female nurse died in a private hospital in Delhi. Nursing staff are protesting over the lack of PPEs (personal protective gear), and demanding a reduction in duty hours. It is alleged that the nurse contracted the infection because health care givers, especially nurses, are forced to re-use PPEs. It is also said that nurses are the most affected among frontline healthcare workers. How do you explain this vulnerability?
UD: Nurses form the backbone of the curative mechanism, i.e. taking care of patients. Once diagnosis is done and a case-sheet is written, nurses take over the task of actual care-giving. And it is the nurse who is in direct contact with the patient through the day and that is where the maximum burden of care-giving falls on nurses.
But, in Intensive Care Units (ICU) or when a patient is put on ventilator, one can see the continuous presence of doctors as well. Overall, it is nurses who form the core of the care-giving mechanism everywhere.
After people stranded in various parts of the country and abroad started returning, the number of infected has gone up slightly in Kerala. We have 15 healthcare givers who have been found positive.
The efforts of the Left Democratic Front (LDF) government in Kerala in fighting the pandemic have been acclaimed worldwide. Health care-givers, especially the nursing staff, are at the forefront of this fight. How did you manage?
The first communist government in Kerala was formed in 1957 under the leadership of EMS Namboodiripad. Rejuvenating the public health system of Kerala was one of the major tasks that the government undertook. In fact, the vision for a people-oriented healthcare system was in discussion a year before the EMS government came into existence.
So, the consistent people-oriented planning of all the successive LDF governments, along with various social institutions and mass organisations that we are part of, together make sure that health remains a people’s issue.
Basically, enormous emphasis is given to State-backed collective efforts. This mechanism also formed the backbone of the public health system that helped Kerala deal with the pandemic as a society. Also, we benefitted from our previous experience during the outbreak of the Nipah virus.
Can you also tell us about the experience of Nipah?
Because of the previous outbreak of the Nipah virus, we already had a protocol in place. That is the reason we could deal with this pandemic situation since the very beginning.
Three members from the same family got themselves admitted in a private hospital in Kozhikode district of Kerala with symptoms of viral infection. The doctors from the virology department of Kozhikode Medical College were called for consultation by doctors of the private hospital where the family was admitted. It was detected as infection from the Nipah virus.
Unlike COVID-19, patients suffering from Nipah virus can affect others only in the stage of acute illness. So, hospitals were the epicentres from where the disease could spread. In fact, a dear colleague, Liny sister, died around this time last year after she contracted the infection while performing her duty.
A protocol of identification, tracing contacts and isolation was also developed at the time of Niph virus. Nurses and cleaning staff received minute training in wearing and removing PPEs etc. during that time. So, when the first patient, a medical student from Wuhan arrived in Kerala on January 30, we were absolutely prepared to deal with the situation.
Also, past experience helped us in spreading medical awareness. If a government conveys the gravity of a medical emergency, the society collectively pays attention and shares the responsibility. Because of the development of this kind of organic link between the government and different tiers of the society, we are in a position to even deal with the revival or community transmission of the virus, if that happens.
Around six lakh families are registered with the state health website after returning to Kerala, and we can institutionally quarantine them if required. Also, the Supreme Court’s guideline is there that recommends for home quarantine.
Can you describe the state healthcare system of Kerala?
In Kerala, we have a very efficient yet decentralised and people-oriented public healthcare system. There are five tiers of government hospitals -- Primary Health Centres (PHC), Family Health Centres, Community Health Centres, Taluk Hospitals and Medical Colleges at the apex of this structure.
Recently, through a project called Ardram, the Kerala government created 700 Family Health Centres by converting the Community Health Centres. So, there are conscious and strong attempts being made for further decentralisation.
Junior Public Health Nurses (JPHN), known as auxiliary nurse midwife or ANMs in other parts of the country, form the backbone of this decentralised healthcare system. In most other states, ANMs are virtually there for namesake. But, in Kerala, the JPHN, along with Junior Health Inspectors, Health Inspectors, Lady Health Inspectors, Mother and Child health Officers are extremely important of the cadres.
The ASHA (Accredited Social Health Activists) workers and the Anganwadi teachers are also an indispensable part this decentralised mechanism. They are the ones who actually have the most organic link with people on daily basis. They create the database required for the effective functioning of the health system, along with spreading awareness regarding public health, i.e. malnutrition and so on.
A JPHN visits pregnant women at least thrice during the nine months. They are the force that informs the state government, through the various categories of junior nurses, about any kind of health emergency. So, all of them are extremely important from the point of view of preventive healthcare.
Then comes the role of the General Nurses and Midwives (GNMs) involved in providing the curative part of. This is an area where I have devoted 33 years of my professional life. Currently, 20,000 nurses are employed in the government sector and two lakh in private hospitals. The tireless efforts of the nurses involved in the curative part of medical set-up should also be acknowledged, as they are the most vulnerable section in a situation like this.
How effectively did ASHA workers perform during this pandemic?
As I said, the role of primary healthcare-level nurses along with ASHA workers and Anganwadi teachers, is extremely important in a decentralised system like ours. ASHA workers get basic training but they are the ones who collect data; if there is any significant fluctuation or emergency kind of situation, they inform the nurses posted in PHCs. Without their input, the system cannot function smoothly.
In a pandemic situation, where awareness building and preventive mechanism are very crucial to stop the spread of the infection, ASHAs played a very important role. But this section of our society that is highly underpaid. The LDF government has announced a hike in the honorarium for ASHA workers, given their contribution during the pandemic, but there is still a long way to go.
I would also like to mention that participation of various social/public institutions, like the Kudumbashree self-help groups run by women, organisations like the Democratic Youth Federation of India and so on, such as in running awareness campaigns, providing relief and other essential services to all sections of the society, without whom the burden on healthcare sector would have been exhaustive.
The Kudumbashree women not only prepared food for a large number of people, but also made masks and hand sanitisers that were distributed to people. The role of the police should also be acknowledged. But, without a decentralised health system being in place and the active participation of the people, wining this battle would not have been possible. So, it is a collective effort that helped not only flattening the growth of infection but also making the recovery rate high and mortality rate low.
There have been many efforts to privatise the healthcare sector of Kerala in the past, when the Congress-led United Democratic front of UDF was in power, such as the previous UDF government’s attempt to sell the super-speciality hospitals of Kerala to a Sharjah-based private group. But this move was resisted by Left-leaning trade unions and various mass and social organisations. So, there is also a history of struggle that is linked with the success of Kerala in combating the pandemic.
Why did you choose this profession?
I always wanted to become a nurse. My mother was admitted to hospital once when I was a child. I was deeply moved by the care that nurses took of her. The compassionate and humanitarian side of the profession inspired me.
Also, the economic condition of my family was another reason and that is the story of the majority of nursing staff of my generation. Many nurses belong to extremely poor families. So, immediately after completing the class X board exam, we got ourselves registered in the course. The government training centres offer courses for free. I did not have to pay any fee. On the top of that I received a Rs 100 fellowship every month.
Immediately after finishing the three-year course, one can register for employment. In fact, many Kerala women opt for this profession primarily for these very (government help) reason. This ensures that the material condition of the family would eventually change.
The gendered nature of the profession also ensures that women face less competition. Historic factors, like the presence of Christian missionaries and their role in the care-giving work, is also another factor. Till date, many Christian women go for our profession. They are the ones who entered the profession initially, which later became popular for social and economic reasons.
Since when have you been in the leadership of this organisation? Can you share some of your experiences in organising nurses?
Given the gendered character the profession, women do come into the leadership position, too. I became president of the Kerala Nurses and Mid-Wives’ Council last year. Previously, I was general secretary of the Kerala Government Nurses Association for two terms (2016-2019) and President (2012-2015).
One of the major hindrances that I have faced in organising nurses is the restrictions imposed on women’s mobility by society, and Kerala is no exception. Getting women to do any kind of organisational activity after 4 ‘0’ clock in the evening, is very difficult. Of course, there are several female nurses who move across districts for organisational work, but for the majority of the members this is not that easy. Roaming outside after dark, for whatever reason, is not socially acceptable yet. This is a big barrier that we need to cross.
How many male nurses are there in different grades? Can you please give us a brief picture of the gender ratio and division of work? Are they also part of the organisation’s leadership?
Since 1979, male professionals started entering the cadre. Then in 1983, the Congress government led by Chief Minister K Karunakaran rolled back this law. Then, in 1988, there was a protest and finally the LDF government brought back the 2% male nurses norm, which became 5% and gradually increased. Now, they comprise almost 20% of the profession.
Of course, there are male nurses in the leadership and even the current head of the Kerala Government Nurses Association is a male, named Subramaniam.
Currently, how many nursing staff are employed in different grades, i.e. nursing superintendent, GNM, ANM etc.? What is the difference in their professional skills and payment structures in the government set-up?
There are about 20,000 nurses in the public sector of Kerala. Around 14,000 are in the public service commission and the rest are in different schemes, like Rashtriya Swasthya Bima Yojana, Directorate of Medical Education, National Health Mission, KHRWS etc.
In the government set up, nurses earn a very decent salary. But there are about two lakhs nurses employed in the private sector in Kerala and for them even getting a minimum salary of Rs 20, 000 a month is very difficult. There is a Supreme Court ruling that mandated the private sector to pay the minimum salary of Rs 20, 000 for the nurses. However, the managements fail to follow this ruling.
There are about 4,800 higher posts in the public sector where nurses can get promoted, such as grade 2, grade 1 nursing, head nurse etc. There is general nursing superintendent grade 2. Above them there three key higher posts, i.e. Director of Health services and Deputy Director of Health Services. In the medical education department, there are about 600 teaching posts. The highest post in the latter is the joint director of medical services.
The promotion of nurses based on experience in the professional field, is quite streamlined. Technically, nursing staff can go up in the higher level of administration but in reality, we see very few getting that opportunity. And at the level where policy decisions are being made, nurses do not have entry at all.
How many government nursing training centres are there in Kerala and how does one get registered for the course, i.e. state level combined entrance test? Is there any difference in the fee structures between government and private training schools?
The general nursing and midwifery course in Kerala has a three-year duration. There are 19 such colleges. BSc nursing is available in all 12 medical colleges of the state. And M.Sc nursing is available in six medical colleges.
Both private and public sector together have 234 nursing schools and 224 nursing colleges in Kerala. Earlier there used to be entrance examination for B.Sc and M.Sc nursing courses, but these do not take place anymore.
Private colleges charge Rs 65,000 per year for B.Sc. nursing and Rs 25,000 for GNMs. However, there is variation in fee among private colleges. Kerala has for long been supplying a vast pool of nurses not only to other states but also to other countries? Is this because they get better remuneration and working environment elsewhere?
A majority of nurses study in Kerala but go outside primarily for better remuneration. If we take into consideration their material condition in totality, the aspiration to go abroad and live there is also there. Perhaps, now to some extent, that is one of the major reasons why women are taking up this profession. The material condition of the families is also one reason. Also, historically, migration of Kerala nurses abroad has been due to various reasons. This has created a demand for nurses trained in Kerala. In many countries they are even known as ambassadors from Kerala.
A large number of nurses have over eight-hour work shifts, including night shifts. There is added burden of household activities. Do you think there is need to address problems in their social life?
It was very difficult earlier, when there were about three months of night duty. This was slowly reduced to one month, and then 15 days, seven days, and when I was general secretary, it was reduced to three days (2017).
In effect, night duty comes to about 12 hours because of the calculation of duty timings, shift change etc. Otherwise 8-hour duty is what most nurses do in three shifts. But, on the whole, the scenario has improved now in the public sector.
Nursing as a profession is heavily gendered where ‘care-giving’ as a woman’s responsibility has been naturalised historically. Do you think this attitude creates structural disparity within the overall care-giver cadre in various forms, like huge payment disparity between doctors and nurses, or other forms of workplace discrimination?
Even though care-giving is seen primarily as a woman’s profession, in a hospital set-up, there are a large number of people who are involved. In hospitals, both male and female nurses take care of bed-ridden patients.
But, there is a huge disparity in the payment structure between doctors and nurses. Here, I am talking about public hospitals. Salary has not increased for nurses as much as it has increased for the doctors. What is more unfortunate is that it takes a pandemic to even acknowledge the presence of nursing staff as professional care-givers.
(The writer would like to thank Deepali Aparajita and P V Aniyan for their inputs for this interview and Gayatri Balusa for help with the translation.)
Get the latest reports & analysis with people's perspective on Protests, movements & deep analytical videos, discussions of the current affairs in your Telegram app. Subscribe to NewsClick's Telegram channel & get Real-Time updates on stories, as they get published on our website.