Mutant Variants of Coronavirus in India: What we Know So Far
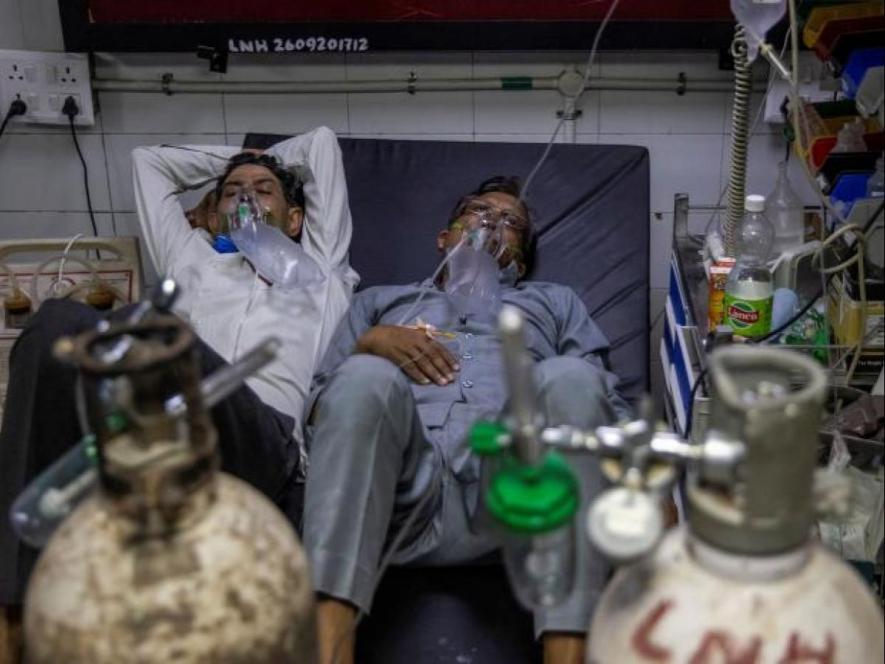
Image Courtesy: Reuters
India is still in the grip of a rampant second wave of COVID-19, with the rapid surge in cases spreading to newer regions from its initial epicentres in Maharashtra, Delhi, UP and Gujarat. Amidst an unprecedented health crisis, scientists and researchers are also busy enumerating attributes that could have caused severe and critical conditions among patients.
One such reason is the emergence of mutant variants of the novel coronavirus. India has several of these variants in circulation in different regions. Genomic data revealed that the B.1.1.7 variant, which first emerged in the UK, was dominant in Delhi and Punjab. Similarly, a new variant named B.1.618 was found to be present in West Bengal, while the B.1.617 or the ‘double mutant’ variant was dominant in Maharashtra.
Within a short span of time the B.1.617 variant became the dominant one across India, reportedly spreading to 40 other countries, including the UK, Fiji and Singapore. Two days ago the World Health Organization (WHO) had also designated it as a ‘variant of concern’. Variants are categorised in such a way when there is evidence that they spread more rapidly, cause serious disease and can evade the immune system better than other variants in circulation.
There are several other variants which have had a significant impact. Studies suggest that the Oxford–AstraZeneca vaccine is less effective against the B.1.351 variant, which was identified in South Africa last year. Similarly, the P.1 variant, which caused a major second wave in Brazil, could evade our immune system. Again, we have the B.1.1.7 variant which emerged in the UK, which led to a surge in cases there and in many other countries.
Coming back to Indian scenario, is the variant of concern – B.1.617 – more transmissible than others? Shahid Jameel, a virologist at Ashoka Univesity, was quoted saying: “Its prevalence has increased over other variants in much of India, suggesting that it has better ‘fitness’ over those variants”.
THE B.1.617 VARIANT AND EMERGING EVIDENCE
The B.1.617 variant was first detected by Indian scientists in October last year. The Indian SARS-CoV-2 Genome Sequencing Consortia (INSACOG) began increasing genomic surveillance in response to a rising number of variants. By mid-February, it was found that B.1.617 represented about 60% of the cases in Maharashtra.
A detailed genomic and structural analysis of the variant was published in the pre-print server bioRxiv on May 3, when scientists from the NIV (National Institute of Virology) identified eight mutations in the spike protein of the coronavirus. Two of these mutations were found to be similar to other mutations that allowed other variants to become more transmissible. A third mutation resembled a mutation present in the P.1 variant which allowed it to partially evade our immunity.
Days later, a team of Germany found that B.1.617 is better at entering the human intestine and lungs in comparison to earlier variants. The team conducted experiments on the human lung and intestine cells grown in a laboratory. They published their findings in bioRxiv on May 5.
Again, on May 5, a team from NIV published a paper in bioRxiv where they reported finding that hamsters infected with B.1.617 had more inflammation in their lungs as compared to animals infected with other variants.
Another team found that antibodies against the B.1.617 variant were slightly less effective as compared to other variants. The researchers published their data in bioRxiv on May 9. What the team did was collect blood serum from nine participants who were immunised with the Pfizer vaccine, and tested it with another harmless virus modified to contain the spike protein with the same mutations present in the B.1.617 variant. The reason for collecting blood serum was that the serum of vaccinated people contains neutralising antibodies against the virus.
The team found that the antibodies of vaccinated people were around to be 80% less effective against some of the mutations present in the B.1.617 variant. However, it would be incorrect to say that vaccines are ineffective against the variant. The researchers also found that some health care workers in Delhi who were vaccinated with Covishield, the Indian version of the Oxford-AstraZeneca vaccine, were re-infected largely by the B.1.617 variant.
The German team also tested serum samples from 15 participants who were previously infected by the coronavirus and found that the antibodies were 50% less effective against the B.1.617 variant in comparison to previously circulating variants.
However, there remain some caveats in such studies, which simply give provide prelimnary indicators that cannot be accepted as conclusive. Scientists caution that serum studies are not always conclusive in saying whether a variant can evade immunity in a real-life situation. The same is the case for vaccine efficacy against variants. Vaccines produce large quantities of antibodies and also stimulate other parts of the immune system, like T cells. A decrease in potency in the antibodies may not be conclusive enough to say that a vaccine does not work effectively against a variant.
An NIV team tested Covaxin against B.1.617 and found that the vaccine worked. The team, however, observed that there is a small drop as far as the effectiveness of the neutralising antibodies produced by Covaxin was concerned.
Get the latest reports & analysis with people's perspective on Protests, movements & deep analytical videos, discussions of the current affairs in your Telegram app. Subscribe to NewsClick's Telegram channel & get Real-Time updates on stories, as they get published on our website.
























