Is India’s Public Healthcare System Equipped to Deal with Coronavirus?

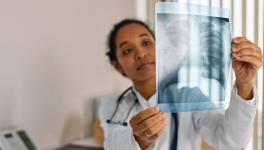
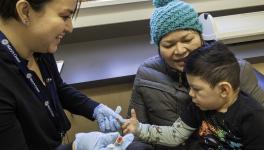
Image for representational use only.Image Courtesy : The Print
As the number of coronavirus (Covid-19) infected people has jumped to 28 as of Wednesday evening, all eyes are on Indian public healthcare system. The question is whether the system is equipped to deal with this issue in case of an emergency?
With the spread of the virus, the central government on Tuesday directed all incoming international passengers to declare their travel history and whether they have come from any coronavirus affected countries to health and immigration officials at the airports across the country. Also, all the international passengers have to go through a thermal scanner irrespective of the country from where they are coming in.
“We are doing better in terms of restriction in the point of entry. However, it will be successful only to an extent. It is partly good luck so far, many people who are coming from outside will not be picked up by the thermal scanners at the airports. This is because they don’t necessarily have a fever,” Dr. T Sundararaman of People’s Health Movement (PHM) told NewsClick.
Screening and precautions are being taken at all possible levels. But pointing out the glitches in our public health system, Dr Sundararaman said, “If the “virus comes and establishes transmission within the population, then we will predictably have 2% of people requiring ventilation. This 2% ventilation is too large a number for us to manage, because we have got huge scarcity in terms of providing tertiary care in district hospitals.”
Also read: Coronavirus: 6 Cases 'High-Viral Load' Detected in Agra
According to the National Health Profile 2019, India has as many as 25,778 government hospitals. Of this, 4,375 hospitals are urban hospitals and the rest 21,403 are in rural India. However, the 21,403 hospitals in rural Indian contain only 2,65,275 beds. Whereas the 4,375 hospitals in urban India have a total of 4,48,711 beds. This accompanied by the population distribution of the country,
shows a dismal picture.
As per the 2011 census, the total population of the country is 1,210.8 million where 31.14% of the population lives in urban areas and the rest lives in rural India. If we compare the population distribution and number of beds available in hospitals, in rural India which has 68.86% of total population, there are only 37% of the total beds available. While, 63% of the total bed are accessible for urban India which has only 31.14% of total population.
As far as health professionals are concerned, a study conducted by a group of scientists in 2019 says that there is a shortage of an estimated 6,00,000 doctors and 2 million nurses in the country. “In India, there is one government doctor for every 10,189 people (the World Health Organisation (WHO) recommends a ratio of 1:1,000), or a deficit of 600,000 doctors, and the nurse:patient ratio is 1:483, implying a shortage of two million nurses,” the study said.
Also read: How Serious Is the Threat of Coronavirus
“If we breach the primary prevention level and transmission within the community is established, then we will be in deep trouble. We must remember that the H1N1 mortality rate is 0.1%, and coronavirus mortality rate is 2%, which means corona has 20 times the mortality rate of flu. Though the mortality rate of 2% is small, the absolute numbers will still be high. We are not really equipped to manage the district hospitals and PHC (primary health centre) level care that we need and, once a sort of complication develops, then we won’t be able to manage,” Dr. Sundararaman said.
“India’s experience of battling against HIV/AIDS, Polio and Nipah has been well-praised. This shows that if our health system prepares enough, it can definitely tackle coronavirus too,” said Dr Amir Ullah Khan, a senior fellow at Rajiv Gandhi Institute for Contemporary Studies (RGICS), adding, “But, of course, the efficiency would be different depending on the states.”
“The recent battle that Kerala won against Nipah gives hope. Of course, Kerala is not Uttar Pradesh, and the success there cannot be easily generalised,” Dr. Khan said.
Highlighting the need for a more intensive system to tackle the zoonotic virus that has claimed the lives of more than 3,000 people across the world, Dr Sundararaman explained, “People have been acting responsibly and we have a reasonably good detection mechanism. Most of the people who would have it, that is something like 80 out of every 100 people infected cannot be differentiated from any other cold or light cough. So they will move around in the population not because they have corona, but they have no reason to suspect corona. People who have travelled out the country will think of the possibility of corona. If one comes from Pondicherry, she/he has no reason to think of corona. So I would say the most dangerous period is the two months period from now because we do need to step up the quality of secondary and tertiary level care. The possibility of delayed peaking of coronavirus is very much possible.”
Also watch: Are We Staring at a Novel Coronavirus Pandemic?
Get the latest reports & analysis with people's perspective on Protests, movements & deep analytical videos, discussions of the current affairs in your Telegram app. Subscribe to NewsClick's Telegram channel & get Real-Time updates on stories, as they get published on our website.