Lockdown is an Important Step to Stop Spread of Coronavirus: Guleria
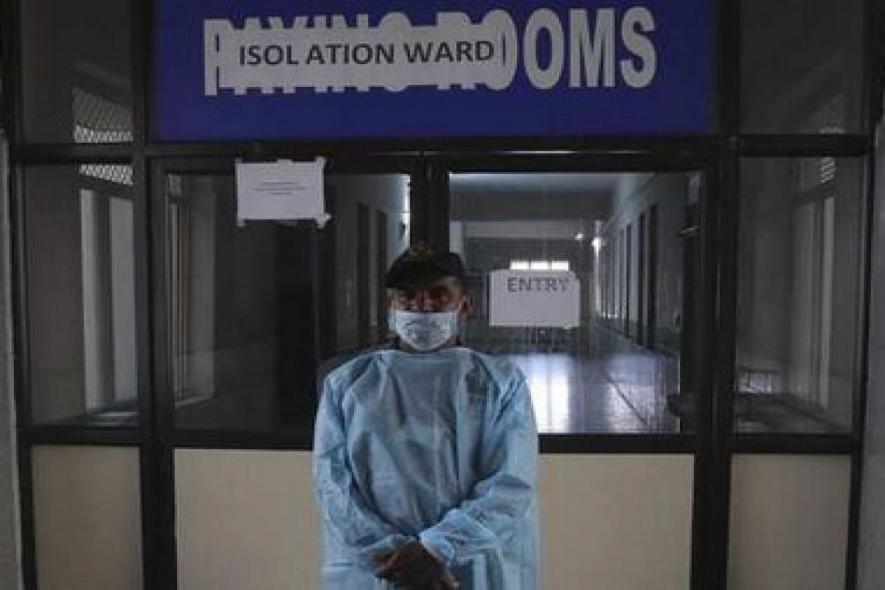
Image Courtesy: First Post
As the Novel Coronavirus, or COVID-19 has spread around the globe, it has also extended its footprint to India, infecting 83 so far and causing two fatalities. Padma Shri awardee and well-known pulmonologist Dr Randeep Guleria, a director at the All-India Institute of Medical Sciences or AIIMS, is overseeing India’s fight against this highly contagious virus. He tells Rashme Sehgal about how this is being done, and why despite social and economic costs, a lockdown alone can stop the disease from becoming a huge burden on India’s healthcare.
The WHO has declared COVID-19, which has spread to 147 countries, a pandemic. What are the implications for India and the world?
The number of infected people is rising steadily. COVID-19 now has a community spread and is occurring in North America, Europe and Asia. Earlier, it had occurred among people who had travelled and those who had come in close contact with them. But this is no longer the case.
The World Health Organisation (WHO) figures of total infections, until Thursday evening, recorded 1,20,000 cases [now 1,46,236]. Different countries are going through different stages of the disease.
The community spread in countries like Iran, Italy and South Korea has shown an increase and this has come from individuals who have not come in close contact with confirmed cases. It is when there is a community spread that it becomes a source of great concern. We know that a large number of such clusters have developed in Italy where people who have not travelled have got infected.
In India, all current cases are of those who have travelled abroad and got the infection or those who have come in close contact with them. This is the first step. We have to stop it from racing ahead. In Europe and the US, a chain reaction has been created whereby it has spread amongst the local people.
Already over 1,500 people have been kept under observation with those who have come in contact with these 74 positive tested so far while another 30,000 are under community surveillance.
In India, so far, we have been able to contain secondary and tertiary transmission of the virus.
The Indian government has imposed strict travel restrictions. Why were these necessary?
In India, we have been able to quarantine a large number of cases. Clusters of illness have not been able to develop as of now because several containment measures have been introduced. Not only are we tracking all the individuals who are suspected of acquiring the disease, so that they can be quarantined for a minimum of two weeks, but we are trying to find out the names of all those these individuals have come in contact with, so that they too can be tested and quarantined.
Is this being done by the health authorities?
Tracking down of individuals is being done by state governments. The district magistrate and other authorities are regularly following this up and educating people. So far, 75 people have come in from abroad [with infections].
It is for this reason that we have cancelled all visas, especially for those who are coming from countries where infections have been reported.
Who is bearing the cost of treatment for those affected?
The state governments are bearing this cost.
This is the first pandemic in many years...
No, the Spanish flu of 1918 was a pandemic. The H1N1 of 2009 was a pandemic. SARS, however, was an epidemic.
Has the Novel Coronavirus been around for a long time or is it a new virus?
The coronavirus has been around for a long time. Ten to 20% of individuals have it, but we have developed immunity to it.
But COVID-19 or Novel Coronavirus is a new virus. Mankind has never been exposed to it before. An animal virus has jumped species and the new virus has the ability to move from human to human.
It has the potential of spreading quickly but its morbidity remains very low. Some 97% of individuals who have it, will recover while 80% will only have mild influenza [after being infected].
But is the Novel Coronavirus more fatal than the common flu?
The mortality rate of COVID-19 is much higher than that of common flu, but much lower than the mortality rate of SARS. There are other forms of coronavirus. We have the MERS or the Middle-East Respiratory Syndrome Coronavirus, and we have been witnessing sporadic attacks of it in West Asia since 2012, but it has not become a pandemic. MERS has a high mortality rate of 30% and is of camel origin. It is also a case in which a virus has jumped species.
Why did Coronavirus jump species in China?
It is difficult to say. It could be due to overcrowding. When a virus in an animal comes in close contact with a virus from a human being, virus reassortment takes place. A new or “novel” virus has developed to which mankind was never exposed before.
Also, earlier disease outbreaks would take time to spread. Now they can span the globe in less than 24 hours and an infected person can spread the virus across several countries. COVID-19 has a long incubation period, of two days to a week. So, in 14 or 15 days it can spread all over the world. It is also an asymptomatic disease.
The first three Novel Coronavirus patients in Kerala [who were infected in Wuhan, China] had mild symptoms and have been discharged. Very few patients in India have gone on to develop pneumonia and the acute respiratory distress syndrome.
Where have these acute cases been admitted?
The cases with severe symptoms are in Intensive Care Units or ICUs and two have been admitted in a Rajasthan Hospital in Jaipur.
If we look at the details from China, we find that 80% of the infected had only mild illness, 15-20% required hospitalisation while 5% were admitted into an ICU. This is an extremely infectious disease and, of course, if you have a huge outbreak, 5% may need ICU. If that were to happen in a country like India, it would be a huge number indeed.
In Italy, they have around 5,000 patients from which more than 1,000 have needed ICU care. Our medical services are already over stretched and we need to be really careful. That is why it is important for us to do aggressive monitoring.
In the United States, clusters of the outbreak broke out in Seattle but then they had started testing for infections rather late.
Do virus attacks have to do with the natural environment and habitats being denuded?
Caring for the environment is very important but excessive overcrowding in small areas is a matter of special concern. Ebola, H1N1 and SARS are all relatively new viral infections. That is why we need to be more vigilant and to develop protocols that can handle subsequent outbreaks.
Is that why such strict travel restrictions have been put in place even though these will affect every sector of economy?
This has huge social and economic costs, but everything must be kept in abeyance while we handle the costs in terms of morbidity and mortality. It is for this reason that meetings and conferences have had to be postponed and tourism has come to a halt. A lockdown is an important step to prevent infection.
Get the latest reports & analysis with people's perspective on Protests, movements & deep analytical videos, discussions of the current affairs in your Telegram app. Subscribe to NewsClick's Telegram channel & get Real-Time updates on stories, as they get published on our website.