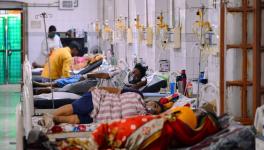
Reactions to COVID Vaccines: Majority Maybe a Nocebo Effect
Much had been talked about the reactions after taking the COVID vaccines, like fatigue, headache, malaise, fever-like conditions, etc. In some cases, concerns about severe reactions have also been raised. Scientists and researchers raised questions about the reactions. Are all of them really due to the vaccines' ingredients, or were there psychological factors involved as well?
Large cohort analysis has been published recently, suggesting that most of the reactions or feelings of the reactions may be psychological. A new study published in the JAMA network involving 45,000 patients indicates that the adverse reactions people experienced after being administered the vaccines are due to the nocebo effect.
Nocebo effect is opposite to placebo. In a placebo, patients are made to believe that they have been given treatment, but no treatment is provided in reality. For example, there is always a placebo group in vaccine clinical trials to whom injection is given, but that does not contain any medicine or any such thing. The patient under a placebo feels that he is given a treatment and starts feeling better. Nocebo is the opposite of it. A person is given an injection or treatment, which does not have any adverse effect, but the person getting it feels having such adverse effect after the injection.
The new study showed that adverse effects were reported by those in the placebo groups of the vaccination programmes. The study analysed 12 randomised placebo-controlled clinical trials of the COVID vaccines and found that 64% of adverse effects were attributable to such nocebo effect.
Julia W. Haas of the Beth Israel Deaconess Medical Center (BIDMC), Boston, USA and a co-author of the research, said, "Adverse events after placebo treatment is common in randomised controlled trials."
Julia Haas is a placebo researcher. "Collecting systematic evidence regarding these nocebo responses in vaccine trials is important for COVID-19 vaccination worldwide, especially because concern about side effects is reported to be a reason for vaccine hesitancy," she further commented.
The 12 clinical trials that the research team studied included 45,380 patients. Out of these, 22,802 were given actual vaccines, and the remaining 22,578 were on a placebo. These patients were entirely in the dark whether they were given the actual vaccine or a placebo (like saline water instead of vaccine). After the first dose, 46.3% of the vaccine patients reported systemic adverse effects, which affected the entire body, including headache and fatigue. Again, 66.7% reported local adverse effects, for example, soreness or swelling at the injection spot.
Again, the people in the placebo group also reported to have experienced adverse effects, and 35.2% of them reported systemic effects while 16.2% had local effects. The team of researchers found that in total, after comparing the two groups, 76% of those reported to have experienced the systemic adverse effect and 24% with local adverse effects had the Nocebo effect. This is the case after the first dose, the researchers concluded.
However, till the second dose was given, these numbers dropped. Fewer placebo patients reported to have experienced adverse effects—31.8% for systemic and 11.8% for local. On the other hand, for the actual recipients of the vaccine, the reported adverse effects went up to 61.4% for systemic and 72.8% for local adverse effects.
Summing up the statistics, the researchers concluded that overall, 64% of all those reported to have adverse effects could be traced down to the nocebo effect.
"Nonspecific symptoms like headache and fatigue – which we have shown to be particularly nocebo sensitive – are listed among the most common adverse reactions following COVID-19 vaccination in many information leaflets," said placebo researcher Ted J. Kaptchuk of BIDMC and Harvard Medical School and a co-author of the study.
"Evidence suggests that this sort of information may cause people to misattribute common daily background sensations as arising from the vaccine or cause anxiety and worry that make people hyper-alert to bodily feelings about adverse events," Kaptchuk added.
Get the latest reports & analysis with people's perspective on Protests, movements & deep analytical videos, discussions of the current affairs in your Telegram app. Subscribe to NewsClick's Telegram channel & get Real-Time updates on stories, as they get published on our website.