Removal of Toxic Substances From Brain Depends on Quality of Sleep
Image Courtesy: medicalxpress.com. Image for representational use only.
When it comes to cleaning the toxic substances out of the brain, all sleep may not be equal; the deeper the sleep, the more effective the cleaning is. A study published in Science Advances recently has shown that the cleaning system of the brain has a correlation with deep sleep.
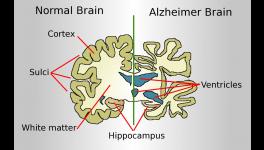
It also reinforces the fact that quality of sleep is related to the development of dementia, like Alzheimer’s disease. In the pathological condition of Alzheimer’s disease, the ability of the brain to remove toxic proteins like amyloid beta or tau fails and these toxic substances accumulate in the brain. With the progression of age, sleep often becomes increasingly lighter and disruptive. This study also potentially explains the links between aging, sleep deprivation and risk of Alzheimer’s disease.
"Sleep is critical to the function of the brain's waste removal system and this study shows that the deeper the sleep, the better it is," said Maiken Nedergaard, Center for Translational Neuromedicine at the University of Rochester Medical Center (URMC) and lead author of the study. "These findings also add to the increasingly clear evidence that quality of sleep or sleep deprivation can predict the onset of Alzheimer's and dementia."
Glymphatic System- the Cleaning Mechanism of the Brain
It is only very recently that any information about the cleaning mechanism adopted by the brain came to be known. It was in 2012 when Nedergaard—the lead author of the study we are discussing, and his team discovered how the brain cleans the toxic out of it. They named it the ‘Glymphatic System’. This unique system functions in a similar way where debris are removed by water using a hose pipe; with water getting replaced by CSF (cerebrospinal fluid) and the pipe by the perivascular channels. The perivascular space in the brain are the tiny spaces between the veins, arteries and the pia mater—the delicate inner most part of the meninges, the protective surrounding of the brain and the spinal cord.
The glymphatic system removes soluble proteins and metabolites from the central nervous system. It is also involved in distribution of compounds like glucose, lipids, amino acids and neurotransmitters in the brain.
Interestingly, the glymphatic system becomes active during sleep and remains largely non-engaged during the period of wakefulness. This says that sleep is not shutting down of the brain; rather, sleep is another state the brain needs to be in for the waste removal system to be active. Since its discovery, plethora of researches have shown that the functioning of the glymphatic system gets suppressed in several diseases and this failure of the system in turn helps in developing neurodegenerative diseases, traumatic brain injury and also stroke.
The Study
The researchers conducted their study on mice. They applied six different anesthetic regimens on the mice and recorded their brain activity through EEG (Electro encephalogram), cardiovascular activity and the cleansing flow of the CSF through the brain. The reason for choosing anesthesia is due to the fact that anesthesia could emulate the natural sleeping state.
The team observed that when ketamine and xylazine (K/X) combination is applied as the anesthetic agent, the EEG records of the brain closely replicated the slow and steady electrical activity in the brain and slow heart rate associated with the deep non-REM sleep. Also, the K/X combination induces the optimal functioning of the glymphatic system in the mice brain.
The clear outcome of the study is that deep non-REM sleep could induce optimal functioning of the glymphatic system—the waste removal system of the brain. Disruptive and lighter sleeps may not be very efficient in inducing the cleansing mechanism of the brain—increasing the chances of accumulation of toxic substances and thus, developing neuro degeneration.
Get the latest reports & analysis with people's perspective on Protests, movements & deep analytical videos, discussions of the current affairs in your Telegram app. Subscribe to NewsClick's Telegram channel & get Real-Time updates on stories, as they get published on our website.