Kerala Still on High Alert After Nipah Outbreak, But The Worst Seems to be Over

The death of a 12-year-old boy in Kozhikode district in Kerala on Sunday morning, hours after he had tested positive for the dreaded Nipah virus, triggered concerns about the state’s ability to handle another outbreak amid a surge in cases of Covid-19. The state government immediately swung into action, tracing the boy’s contacts and keeping all immediate ones under isolation and close observation. Even as all districts in the state remain on high alert, all 68 samples of immediate contacts that were considered high-risk, including the boys’ parents and relatives, have tested negative for the virus. It indicates that there is no need to panic. With the spread of the virus seemingly contained, the focus now is on finding the source of the infection.
The Nipah Virus
The Nipah Virus (NiV) is a zoonotic virus that can transfer to humans after being incubated by other species. In infected people, it causes a range of illnesses from asymptomatic infection to acute respiratory illness and fatal encephalitis. Fruit bats of the family Pteropodidae are the natural hosts for Nipah Virus and it can pass onto other animals and also infect animals and humans who consume fruits bitten by the infected bats or come into unprotected exposure to their secretions. Human-to-human transmission can occur among close contacts, primarily family and caregivers who come into contact with bodily fluids or respiratory droplets of the infected patients. The incubation period ranges from 4-14 days, but can also be higher in some cases. There is no treatment or vaccine available for either people or animals contracting the virus and the primary treatment for humans is supportive care. The reported fatality rate is between 46-96%.
First recognized in a large outbreak in Malaysia and Singapore in 1998-99, in which 105 deaths were recorded among 265 identified cases, there have been frequent outbreaks of the Nipah Virus in Bangladesh. The World Health Organization (WHO) notes that around half of the reported cases in Bangladesh were due to human-to-human transmission. Prior to the first outbreak in Kerala in 2018, there had also been two other recorded outbreaks in India – in 2001 and 2007 in the Siliguri and Nadia districts of West Bengal, in which over 50 people had died.
The current outbreak in Kozhikode
The infected boy was brought to a private hospital in Kozhikode on September 1, and his fever and vomiting proceeded to bouts of fits and repetitive seizures. The boy also had heart palpitations and detailed checkup revealed major problems in his heart, lungs and brain. Confirmation of all 3 samples collected from the boy testing positive for the Nipah virus was received late at night on September 4 from the National Institute of Virology (NIV) in Pune, and the boy succumbed to the disease within a few hours. His body was laid to rest at the Kannamparamb Khabaristan by Health Department officials and a few close relatives clad in Personal Protective Equipment (PPE) kits, adhering to strict health protocols, in a 12-foot grave.
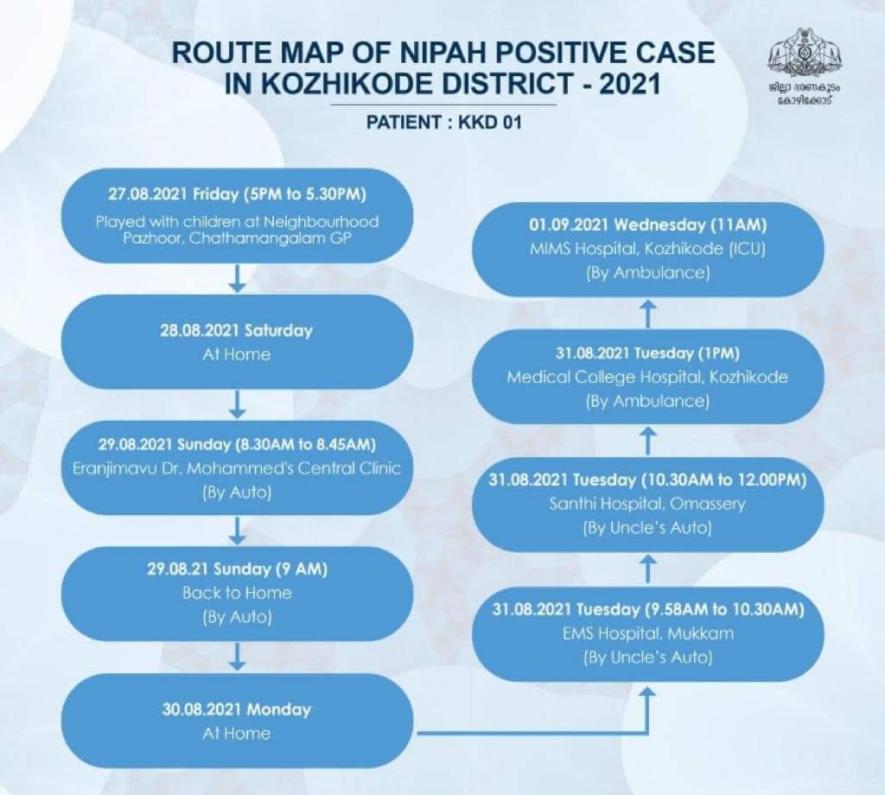
The state government’s response began immediately. 3 wards in Chathamangalam panchayat, where the boy had hailed from, were completely shut down and micro-level restrictions were enforced. A Nipah Management Plan was prepared by the Department of Health and Family Welfare within hours of the boy’s death, along with new guidelines for treatment and discharge. With the aim of effectively preventing the spread of the virus, 16 committees were formed to oversee the monitoring, sample testing, result management, contact tracing, transport for the sick, infrastructure management and data analysis. A route map of the boy’s whereabouts prior to his admission to the private hospital and a contact list were prepared and those close contacts who were identified to be in the high-risk category were transferred to an isolation ward set up for this purpose overnight at the Kozhikode Medical College.
A control room was set up and began functioning on the very next day to coordinate the tracking and tracing activities undertaken by health workers and trained personnel recruited for this purpose. By then, a laboratory was also operationalized at the Kozhikode Medical College with the help of NIV Pune and NIV Alappuzha, wherein samples of contacts could be tested and results obtained within 3-4 hours. Awareness campaigns were started in the regions surrounding the boy’s house and health workers started house visits to collect information regarding possible contact and symptoms developed. An E-health software was also introduced to share all information about the virus and its spread to concerned departments and authorities in other districts. Apart from Veena George, the Minister for Health and Family Welfare, AK Saseendran, PA Mohammed Riyas and Ahammad Devarkovil, who are other ministers from the area, also camped in Kozhikode to oversee the activities.
As of today, there are 274 people in the contact list prepared by the Health Department, of whom 149 are health workers and 47 are from other districts. All of them are under observation, and 68 of them who have been identified as being in the high-risk category have been kept in isolation in Kozhikode Medical College. By Thursday night, all 68 samples collected from the close contacts had tested negative and only 7 people on the contact list are reported to have minor symptoms like fever and headache.
Lessons from 2018 and 2019
When the Nipah Virus was first confirmed in Kozhikode in 2018, Kerala was caught off-guard as it had had no past experience of handling a virus with such a high fatality rate and no known treatment. The disease was diagnosed only after 4 deaths and the state had to scurry and put in place a protocol similar to the one for Ebola Virus Disease (EVD), tracing primary, secondary and tertiary contacts and then isolating and monitoring them. Around 3000 people had to be placed under quarantine at one point and the Health Department had to convince them to ensure compliance. 17 of the 18 infected patients died during the outbreak.
But when the virus reappeared in 2019 in Ernakulam, the state was able to contain the infection to the lone index case (the first case, or patient zero) and there were no deaths. Behind the scenes, the state had been monitoring cases of healthy people being admitted with symptoms similar to that of pneumonia and also sampling and examining encephalitis deaths. Former Health Minister KK Shailaja had won widespread acclaim for the work she and her department had done in containing these outbreaks.
This time around, the state has the added benefit of the strict Covid-19 protocols in hospitals and the use of gloves, masks and PPE kits among healthcare workers, as a result of which the chances of an institutional outbreak are far lower. Moreover, compliance with masking and physical distancing norms is also high in Kerala among the general public. The experience of health workers in intensive contact tracing and surveillance, which the state has been continuously carrying out since the outbreak of the covid19 pandemic in March 2020, has also meant that the state could intervene quickly and effectively. Availability of beds, Intensive Care Units (ICUs) and ventilators could be ensured quickly because of the strong public health system which has not been overwhelmed by the high number of Covid-19 cases.
More work to be done
While briefing the media on Thursday, George expressed relief that all the samples collected had tested negative. However, she insisted that the state would not lower its guard and that all restrictions would remain in force till the window period of 3 weeks is over. Even as panic among the public has died down and the state has restarted its vaccination drive in Kozhikode that had been halted due the Nipah Virus outbreak, the focus is now on confirming that the boy is the index case and finding the source of the infection. Health workers who have conducted a house-to-house survey in the containment zone around the boy’s house have so far found no instances of unusual fever or death in the area.

The Health Department has also collected samples from fruit trees and animals near the boy’s house. The presence of bats in the area has reinforced the suspicion that they have been the sources of the infection, both this time and in the previous two instances. Earlier, samples collected from bats in the area of the outbreak in 2018 had tested positive for the virus strain found in the infected patients. The recurring outbreaks, and the fact that this year’s first case is from an area just 30 km away from that of the index case in 2018, raises concerns about the possibility of more outbreaks and what the state can do to prevent the same. Questions have also been raised as to why infection had not been caught earlier– the boy had visited 4 other health facilities before he was admitted to the private hospital. Preventing future outbreaks will rest on the state finding answers to these questions.
Get the latest reports & analysis with people's perspective on Protests, movements & deep analytical videos, discussions of the current affairs in your Telegram app. Subscribe to NewsClick's Telegram channel & get Real-Time updates on stories, as they get published on our website.
























